Mouse model reveals Parkinson’s disease begins in gut and travels up neurons to brain: Study

Parkinson’s disease starts in the gut, shows new research from Johns Hopkins Medicine. The study, published in the journal Neuron, is the first experimental proof that Parkinson’s disease originates among cells in the gut and travels up the body’s neurons to the brain. Experiments in mice show the transmission of a nerve-killing protein from the gut into the brain. Blocking the transmission route could be key to preventing the disease, the researchers say. They are hopeful that the results of their study could eventually lead to practical methods that could prevent or halt the progression of Parkinson’s.
“The findings provide further proof of the gut’s role in Parkinson’s disease and give us a model to study the disease’s progression from the start. This is an exciting discovery for the field and presents a target for early intervention in the disease,” says Dr. Ted Dawson, director of the Johns Hopkins Institute for Cell Engineering and professor of neurology at the Johns Hopkins University School of Medicine.
Parkinson’s disease is a brain disorder which occurs when nerve cells, or neurons, in an area of the brain that controls movement become impaired and/or die. The disease is characterized by the buildup of a "misfolded" or abnormally folded protein, called alpha-synuclein, in the cells of the brain. “As more of these proteins begin to clump together, they cause nerve tissues to die off, leaving behind large swaths of dead brain matter known as Lewy bodies,” say the researchers. As brain cells die, they impair a person’s ability to move, think, or regulate emotions.
In observations or theories proposed earlier, researchers had suggested the gut-brain connection in initiating Parkinson’s disease. The new study builds off observations made in 2003 by German neuroanatomist Heiko Braak, who had said people with Parkinson’s disease also had accumulations of the misfolded alpha-synuclein protein in the parts of the central nervous system that control the gut. Braak had hypothesized that Parkinson’s disease advanced up the nerves connecting the gut and the brain like going up a ladder.
Accordingly, the current study explored whether the abnormally folded alpha-synuclein protein could travel along the nerve bundle known as the vagus nerve, which runs like an electrical cable from the stomach and small intestine into the base of the brain. To test this, the researchers injected 25 micrograms of synthetic misfolded alpha-synuclein created in the lab into the guts of dozens of healthy mice.
They sampled and analyzed the mouse brain tissue at one, three, seven, and ten months after injecting them. Over the course of the 10-month experiment, the researchers saw evidence that the alpha-synuclein began building where the vagus nerve connected to the gut and continued to spread through all parts of the brain.
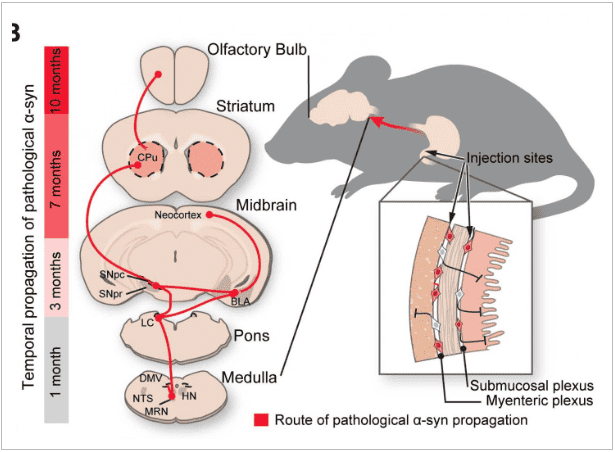
In their next experiment, the researchers once again injected the guts of another group of mice with the misfolded alpha-synuclein. But this time, they surgically cut the vagus nerve. After seven months, the researchers found that this second group of mice with severed vagus nerves did not show any signs of cell death observed in mice with intact vagus nerves. The severed nerve appeared to stop the misfolded protein’s advances, say the researchers.
“The results show that misfolded alpha-synuclein can be transmitted from the gut to the brain in mice along the vagus nerve, and blocking the transmission route could be key to preventing the physical and cognitive manifestations of Parkinson’s disease,” the findings stated.
The researchers investigated whether these physical differences in Parkinson’s disease progression resulted in behavioral changes. They looked at tasks they commonly used to distinguish signs of mouse Parkinson's disease, including nest building and exploring new environments.
“Healthy mice often make large, dense mounds in which to burrow. Smaller, messier nests are often signs of problems with motor control. Seven months after injection, the mice were provided with nesting materials, and their nest building behavior was observed for 16 hours. They were scored in their capabilities on a scale of 0-6. Mice that received the misfolded alpha-synuclein injection scored consistently lower on nest building. In ways similar to Parkinson’s disease symptoms in humans, the mice’s fine motor control deteriorated as the disease progressed,” said the research team.
In another experiment, the researchers analyzed the mice for symptoms similar to Parkinson’s disease in humans, by measuring their anxiety levels and monitoring how they responded to new environments. For this test, the researchers placed the mice in a large open box where a camera could track their exploration.
The researchers say they conducted this experiment as healthy mice are curious and will spend time investigating every part of a new environment. However, they add, mice affected by cognitive decline are more anxious, and they are more likely to stay towards the sheltered edges of the box.
Results show that mice that had their vagus nerves cut to protect against Parkinson’s disease spent between 20 and 30 minutes, exploring the center of the box. On the other hand, mice that received the misfolded alpha-synuclein injection but had intact vagus nerves spent less than five minutes exploring the center of the box and moved mostly around the borders. This, say the researchers, indicate higher anxiety levels, which are consistent with symptoms of Parkinson’s disease.
The research team now plans to analyze what parts of the vagus nerve allow the misfolded protein to climb to the brain, and to investigate potential mechanisms to stop it.
The study was published in the journal Neuron and appeared online June 26.










