Coronavirus pandemic: People with blood type A are at higher risk of infection, finds study

People with blood type A have a significantly higher risk of getting infected with the new coronavirus compared to non-A blood groups. This is the finding of a new study by researchers from China who say that blood type O has a significantly lower risk for infection and severity compared to non-O blood groups.
The study, which analyzed patients in Wuhan, also found that those with type A blood are more likely to die from COVID-19. Of the 206 patients in the study who died, 85 had type A blood, corresponding to 41.26% of all deaths, shows the analysis, a pre-print version of which can be accessed at medRxiv.
So far, over 7,950 people have died in the COVID-19 pandemic and over 198,100 cases have been reported. Current clinical observations suggest that people's age and gender are two risk factors in the susceptibility to COVID-19.
Older people, those with underlying health conditions and men are more susceptible to infection and development of a more severe disease, say experts.
However, no biological markers have been identified to predict the susceptibility to COVID-19 so far, say researchers from China.
Accordingly, the team compared the blood group distribution in 2,173 patients with COVID-19 confirmed by tests from three hospitals in Wuhan and Shenzhen, China, with that in normal people from corresponding regions.
Health experts collected ABO-typed blood samples from 1,775 patients infected with COVID-19, including 206 dead cases, at the Jinyintan Hospital in Wuhan.
Another 113 and 285 patients with COVID-19 were respectively recruited from Renmin Hospital of Wuhan University, Hubei province and Shenzhen Third People's Hospital, Guangdong province, China.
Two recent surveys of ABO blood group distribution of 3,694 normal people from Wuhan City and 23,386 normal people from Shenzhen City were used as comparison controls for the Wuhan and Shenzhen patients with COVID-19, respectively, says the team.
According to the results, the ABO blood group in 3,694 normal people in Wuhan displayed a percentage distribution of 32.16%, 24.90%, 9.10% and 33.84% for A, B, AB, and O, respectively.
The 1,775 patients with COVID-19 from Wuhan Jinyintan Hospital showed an ABO distribution of 37.75%, 26.42%, 10.03% and 25.80% for A, B, AB, and O, respectively.
"The proportion of blood group A in patients with COVID-19 was significantly higher than that in normal people, being 37.75% in the former versus 32.16% in the latter. The proportion of blood group O in patients with COVID-19. was significantly lower than that in normal people, being 25.80% in the former versus 33.84% in the latter," says the team.
They add, "These results corresponded to a significantly increased risk of blood group A for COVID-19 with an odds ratio (OR) of 1.279 and decreased risk of blood group O for COVID-19 with an OR of 0.680 in comparison with non-A groups and non-O groups, respectively."
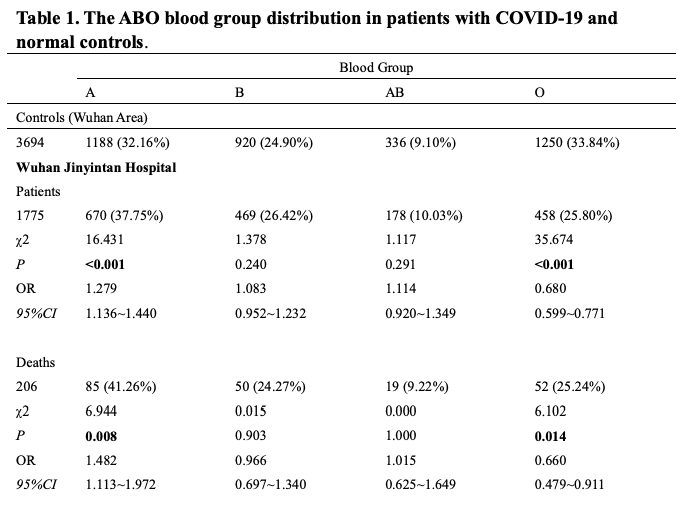
The researchers observed a similar distribution pattern of high-risk blood group A and low-risk blood group O in the dead patients. Specifically, the proportions of blood groups A, B, AB and O in the 206 dead patients were 41.26%, 24.27%, 9.22%, and 25.24%, respectively, say experts.
"Blood group O was associated with a lower risk of death compared with non-O groups, with an OR of 0.660. On the contrary, blood group A was associated with a higher risk of death compared with non-A groups, with an OR of 1.482," says the study.
The second analysis, which examined 113 patients with COVID-19 from the Renmin Hospital of Wuhan University, also had similar results. The analysis shows that 45 (39.82%) patients had type A blood group, the highest in the group.
"Specifically, compared with non-O groups, blood group O was significantly associated with a lower risk of infection. Compared with non-A blood groups, blood group A displayed higher relative risk than those observed in patients from Wuhan Jinyintan Hospital," says the team.
The study further says that the ABO blood group in 23,368 normal people in Shenzhen displayed a percentage distribution of 28.77%, 25.14%, 7.32% and 38.77% for A, B, AB, and O, respectively.
The third analysis of 285 patients with COVID-19 from Shenzhen showed proportions of blood groups A, B, AB and O to be 28.77%, 29.12%, 13.68%, and 28.42%, respectively.
"Similarly, a significantly lower risk of infection was associated with blood group O. Additionally, we found that blood group AB had an increased risk of infection in this group," the findings state.
According to researchers, the results demonstrate that the ABO blood type is a biomarker for "differential susceptibility" of COVID-19. "We, for the first time, report a link between COVID-19 susceptibility and the ABO blood group, demonstrating the latter to be a biomarker differentiating the former," conclude the researchers.
They say that the lower susceptibility of blood group O and higher susceptibility of blood group A for COVID-19 "could be linked to the presence of natural anti-blood group antibodies, particularly anti-A antibody," in the blood.
"This hypothesis will need direct studies to prove. There may also be other mechanisms underlying the ABO blood group-differentiated susceptibility for COVID-19 that require further studies to elucidate," says the team.
The findings have potential clinical implications given the current COVID-19 crisis. The experts recommend that people with blood group A might need particularly "strengthened personal protection" to reduce the chance of infection.
"COVID-19-infected patients with blood group A might need to receive more vigilant surveillance and aggressive treatment. It might be helpful to introduce ABO blood typing in both patients and medical personnel as a routine part of the management of COVID-19 and other coronavirus infections, to help define the management options and assess risk exposure levels of people," says the team.
They, however, add that further studies are needed on this aspect and one should be cautious to use this study to guide clinical practice at this time.